Opioids and Early Death in America
Dartmouth College
The Issue:
Two disturbing trends in the United States have surfaced during the past several decades. First, deaths involving prescription or illicit opioids have taken more than 300,000 lives since the late 1990s. Second, death rates among non-Hispanic white, middle-aged Americans have increased dramatically during the same period, reversing decades of increasing U.S. longevity, and diverging from continued improvements in European countries. While these two trends are closely related in some ways, the opioid epidemic by itself does not fully explain the increases in death rates of Americans at their most productive ages. Neither trend shows signs of moderation and both need to be addressed by effective policy responses.
Increasing drug overdose rates are not the only source driving the rise in mortality for Americans in their most productive ages. Those with lower levels of education and poorer employment prospects are most affected by all causes of rising mortality.
The Facts:
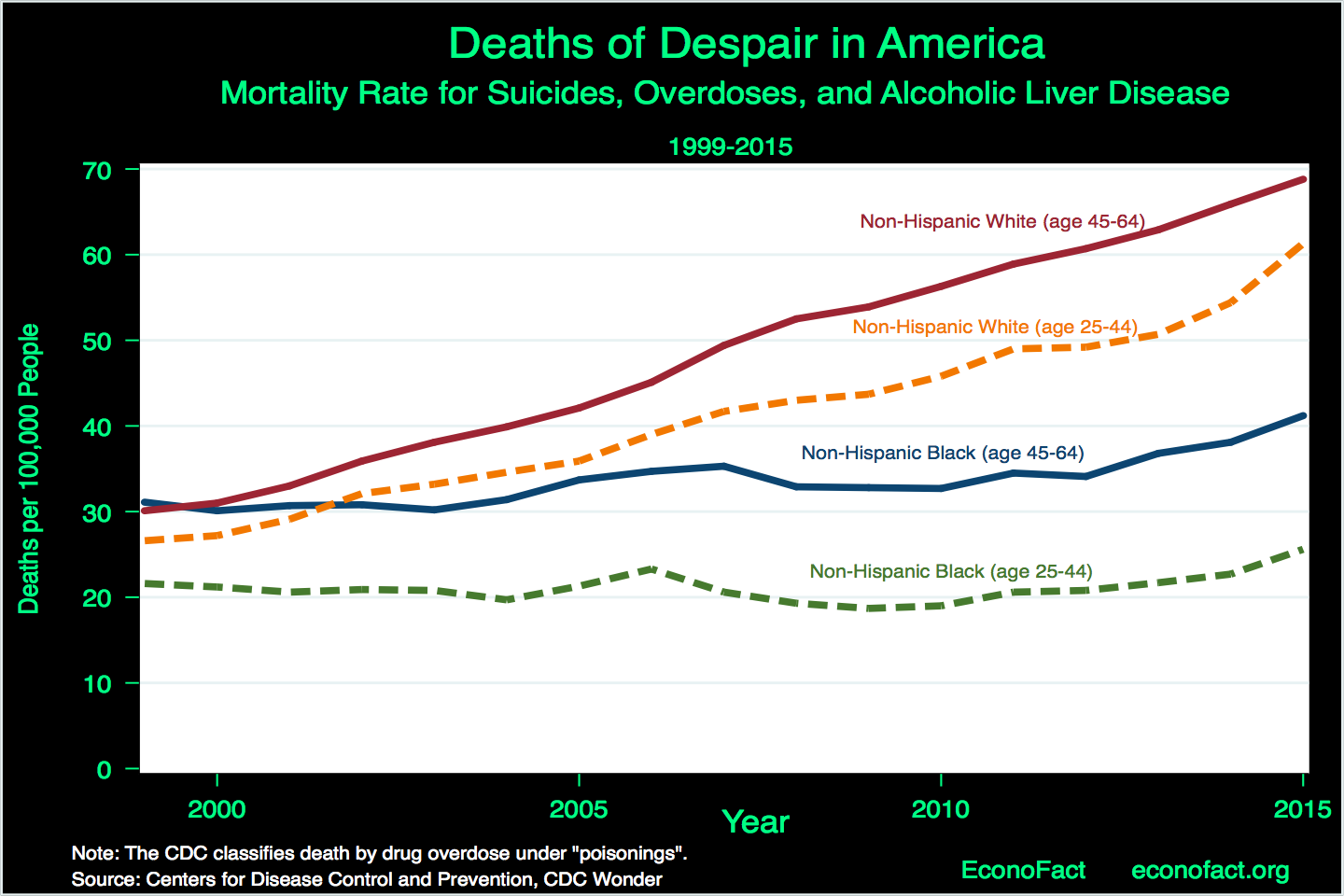
- Opioid overdoses and “deaths of despair” are on the rise for Americans 25-64, but so are deaths from lung and cardiovascular diseases. Economists Anne Case and Angus Deaton have grouped together opioid overdoses with deaths by suicide and alcoholic liver disease to create a broader measure of “deaths of despair,” and these continue to rise at an alarming rate (see chart). Yet other sources of illness among older middle-aged people such as heart disease, stroke and lung disease are are also on the rise.
- Rising mortality is not a problem for kids or older people. By contrast, traditionally vulnerable populations — the oldest and the youngest — are experiencing survival gains. In the poorest counties in the U.S., between 1990 and 2010, the three-year rate of child mortality (deaths per 1000 population aged 0 to 4) nearly halved from 4.49 to 2.29 for boys and 3.61 to 2.04 for girls. In the population aged 65 and older, death rates fell by 10 percent for women and 20 percent for men during the same period. The data demonstrate rising death rates are concentrated exclusively among populations in their peak of productivity, a pattern suggestive of social rather than physiologic causes.
- Although they have been hard hit, the opioid overdose epidemic is not limited to white, Trump-voting men. A 2017 analysis by Case and Deaton revealed the wide reach of opioids. Both women and men of White, non-Hispanic origin experienced similar rises in opioid-related mortality between 1998 and 2015. For example, death rates at ages 50 to 54 increased by over 200 per 100,000 for both men and women with a high school degree or less schooling. Moreover, rising death rates are not confined to middle-aged Americans. For every birth cohort since 1950, death rates at age 40 due to drugs, alcohol, and suicide have risen. The same is true at age 30 for every birth cohort since 1965. Rural and urban areas are both affected. While blacks appeared protected early on, they have experienced rising mortality due to deaths of despair during the 2010-15 years (see chart).
- Low levels of education are associated both with not working and with deaths of despair. One factor common to rising death rates from diverse causes is lower levels of education; those with a high school degree or less are affected most. This is significant because less educated Americans have exited the labor force in historic numbers, and among those still employed, wages are stagnant or falling. Deaths of despair are particularly concentrated in the growing group of people who are not working (or work very little) and depend on the federal Social Security Disability Program (SSDI), a group we estimate dies of opioid overdose at ten times the national rate. A recent analysis suggests county-level opioid overdose deaths per 100,000 increased 0.19 percentage points with each percentage point rise in unemployment between 1999 and 2014.
- Given the broader context for increasing mortality rates, prescription regulations alone are unlikely to fix the opioid epidemic, but might curb its worst excesses. The United States represents less than five percent of the world population and consumes 80 percent of the global opioid supply. Both prescription and illicit opioids contribute to rising opioid overdose deaths. Up to 75 percent of adults treated for opioid addiction report they moved to heroin after starting with prescription opioids, motivated by a lower price and easy access. These disparate opioid sources (pharmacy and street) suggest diverse solutions will be needed. Yet states have focused legal efforts on creating new laws aimed at restricting controlled prescription drugs, an approach with no direct effect on illicit opioids. There is little evidence laws reduced risky opioid prescriptions and overdose for disabled Medicare beneficiaries, a population with high prescription opioid use. However, combinations of distinct laws enacted more recently are associated with lower prescribing and lower overdose death rates in a broader population of Americans.
- Regulating opioids won’t necessarily reduce alcohol abuse or other causes of deaths of despair, nor is it likely to address the less-understood problem of rising cardiovascular and pulmonary deaths. What else is needed? The alarming rise in death rates from opioid overdose is not happening in isolation but rather in the context of rising mortality rates, from diverse causes, for broad segments of the U.S. population. Opioids have contributed to the rise in mortality, but they are not the only source of increasing premature death. The fact that the group most affected by all causes of rising mortality is also more likely to face stagnant employment and wage prospects suggests broader forces contribute to these rising deaths. Determining causality is difficult. Declining wages and employment may make people more susceptible to opioid addiction, alcoholism and suicide. At the same time, addiction and health problems likely make it more difficult for those not working to return to the labor force. And, since many people access health insurance through employment, declining labor prospects might affect people's access to healthcare and their ability to treat chronic conditions. Declaring the opioid crisis a national emergency may ensure resources are allocated to reducing opioid use, but this declaration is not likely to reverse the problem of stagnant or even rising mortality rates. Framing this crisis, in part, as a workforce challenge might invite alignment of two of the administration’s stated priorities: Jobs and a reduction in opioid abuse. If the challenge is to get people back to work, the most direct approach would be expansion of the Earned Income Tax Credit (EITC) as suggested by economist Alan Krueger, particularly to those who haven’t been covered generously in the past such as older workers whose children have moved out, which would have the effect of increasing their after-tax wages.
What this Means:
The current crisis of rising mortality and opioid overdose are part of a widespread deterioration in working conditions that spans (middle) ages, race, and gender, as well as multiple distinct causes of death. Close scrutiny of labor market policies does not deny the importance of getting illegal and legal opioid use under control, which is closely linked to reduced labor supply, nor does it guarantee that other factors leading to poor cardiovascular and pulmonary health will be improved by labor market policies. But expanding labor market opportunities for the cohort of people most affected by rising mortality rates is a great place to start.
Like what you’re reading? Subscribe to EconoFact Premium for exclusive additional content, and invitations to Q&A’s with leading economists.