Pollution, the Flu Shot, and Hospitalizations
University of California, San Diego, Columbia University, Cornell University, and University of California, San Diego
The Issue:
Poor air quality has a lot of negative consequences: it shortens our lifespans, hinders learning, damages our brains, and makes us less productive at work. Environmental regulations are one tool for keeping pollution levels in check, but the 2020 wildfires that raged throughout California highlight the ubiquity of air pollution outside the scope of regulations. There’s emerging evidence to support one surprising action that people can take to help guard against one of the harms from unexpected increases in air pollution: getting a flu shot.
The flu leads to more hospitalizations when there is more air pollution. Vaccination against the flu could mitigate this negative impact of pollution.
The Facts:
- Seasonal influenza is a large and recurring danger in the United States. There are an estimated 25 million to 50 million cases of influenza each year, and the flu accounts for 225,000 hospitalizations and ultimately more than 20,000 deaths yearly. The majority of deaths (>90%) occur among elderly persons, usually those with chronic underlying health conditions. Despite the flu’s large burden, only about half of American adults receive a flu shot each year, far below the 70% target that the Department of Health and Human Services set for flu vaccination rates in 2010. The vaccination protects the person receiving the shot from the flu and also helps reduce virus transmission to others.
- Pollution makes flu season worse by increasing influenza hospitalizations. A number of medical studies suggest air pollution can make individuals more susceptible to respiratory illnesses, including influenza. In our new working paper, we show that periods of worse air quality are followed by periods of increased hospitalizations due to influenza, even after taking into account weather, season, and common regional differences in air quality and demographics. Using the Air Quality Index (AQI), a measure developed by the Environmental Protection Agency (EPA) to describe dangers to human health from poor air quality, we find a clear positive correlation between higher AQI (worse air quality) and the hospitalization rate for influenza. A standard deviation increase in the AQI results in approximately 7,800 additional influenza hospitalizations during flu season across the United States. Given the persistent disparity in exposure to air pollution across U.S. regions, these results could provide one potential contributing factor for the puzzling finding that minority groups in the United States have substantially higher influenza hospitalization rates (see here).
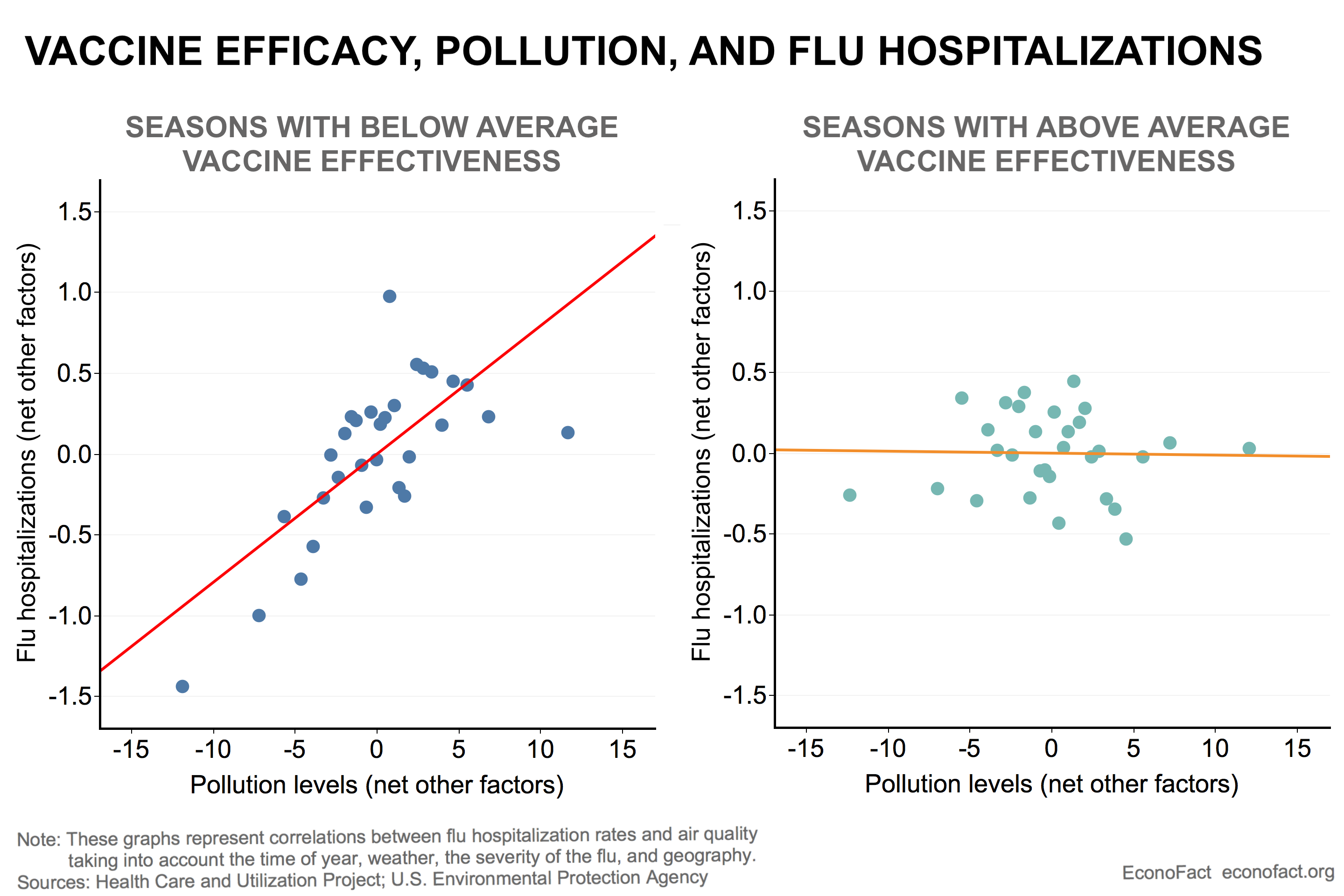
- An effective and widespread flu vaccine can help reduce the dangers of air pollution. If one of the negative impacts of pollution is a heightened risk of hospitalizations from the flu, then vaccination against the flu could mitigate this harm by reducing the spread and severity of influenza. Due to random shifts in the influenza strain, the effectiveness of the flu vaccine varies across years. Since health officials started tracking it in 2003, effectiveness has varied from year to year, ranging from a low of 10% in 2004-05 to a high of 60% in 2010-11 (see here). We find that in years with greater vaccine effectiveness the link between air quality and influenza hospitalizations disappears (see chart). In other words, more effective vaccines negate the effect of poor air quality on influenza hospitalizations. Since the share of people protected by a vaccine is the product of vaccine take-up and vaccine effectiveness, this finding means that higher take-up shares could have the same moderating effect as higher vaccine effectiveness.
- Air quality regulations and vaccine programs are complementary health programs when it comes to reducing flu hospitalizations. Given the random nature of some pollution shocks such as wildfires, and the uncertainty of the annual strain match for influenza, programs designed to improve air quality and increase vaccine take-up can each help hedge against the risk of bad flu outcomes. A back of the envelope calculation suggests a 10% reduction in our pollution measure during an ineffective vaccine year (17% effectiveness) with an average vaccine take-up would avert 16.6% of all influenza-associated hospitalizations across the U.S. Meanwhile a 10% improvement in vaccine take-up at the average vaccine effectiveness (or, equivalently, a 10% improvement in vaccine effectiveness at the average vaccine take-up) in a historically polluted year (38.2 AQI) would avert 34.6% of pollution driven influenza hospitalizations.
- As fire season lengthens and extends into flu season, influenza season will become more hazardous and expensive. Both the length of fire season and its intensity have risen in recent years. The global average fire season has lengthened nearly 20% over the past few decades, and the frequency of large fires in the western United States has increased dramatically since the 1970s, with about 20 additional large fires per decade (see here). Pollution from wildfires has disastrous effects on air quality, which sometimes extend thousands of miles. Air monitor data shows that during the 2020 wildfires, the concentrations for the smallest monitored particulate in parts of the west coast reached 200 micrograms per cubic meter – air quality standards in the United States for such particulates are 12 micrograms per cubic meter. The Air Quality Index was regularly in the range marked "Very Unhealthy" or "Hazardous" (the worst possible ranking) in cities across the west coast. By the end of September when fires had calmed, one could still see the effects on air quality as far as Massachusetts. A longer wildfire season means more overlap with flu season, and thus a likely increase in flu hospitalizations across the country if flu vaccine effectiveness or take-up do not increase.
What this Means:
An extensive literature has shown that improving air quality carries a multitude of benefits. Our results suggest reduced hospitalizations from the flu is yet another. The results also imply that seemingly disparate policy actions of pollution control and expanded flu vaccination provide greater returns to public health than found when studied in isolation. We can improve outcomes through more prolific and effective vaccines, better air quality, or both. Since we cannot fully control the vaccine/influenza match in any given year, investing in air quality controls can help hedge against bad vaccine matches. And since we cannot predict wildfire outbreaks and the shocks they bring to pollution, investing in a robust vaccine infrastructure and widespread take-up can hedge against poor air quality shocks. If getting the flu shot protects us against some of the dangers of air pollution, it gives policymakers one more reason to encourage vaccine take-up in polluted areas, and one more reason for people to go out and get vaccinated. With our healthcare system already under stress due to COVID-19, anything that can reduce additional hospitalizations has high returns.
Like what you’re reading? Subscribe to EconoFact Premium for exclusive additional content, and invitations to Q&A’s with leading economists.